Presentation Summary
Explore Gary Woodland's medical journey from a brain surgery diagnosis to his triumphant comeback in professional golf, detailing his career, diagnosis, surgery, recovery, and the psychological aftermath.
Full Presentation Transcript
Slide 1: Gary Woodland's Brain Surgery Journey: From Crisis to Comeback
A Comprehensive Chronicle of Medical Diagnosis, Surgical Intervention, and Triumphant Return to Professional Competition
Slide 2: Agenda: A Five-Act Medical and Personal Narrative
- Section 1: Gary Woodland's Professional Identity and Career Achievement
- Section 2: The Medical Crisis - Diagnosis and Clinical Discovery
- Section 3: Surgical Intervention and Technical Procedure
- Section 4: Physical Recovery and Return-to-Sport Timeline
- Section 5: Psychological Aftermath and Mental Health Transformation
- Section 6: Competitive Comeback and Broader Implications
Slide 3: Gary Woodland: Professional Identity and Major Championship Status
- Four-time PGA Tour Winner: Elite professional credentials with multiple tournament victories on the PGA Tour
- 2019 U.S. Open Champion: Major championship victory at Pebble Beach Golf Links, affirming elite status in professional golf
- Consistent Tournament Performer: Top-25 finishes across multiple seasons demonstrating sustained excellence and competitive excellence
- Age 39 at Diagnosis: Peak performance years in professional golf career, challenging personal health circumstances at career height
- Family-Oriented with Resilience: Married to wife Gabby with three children: Jaxson, Maddox, and Lennox. Prior adversity includes loss of daughter and twin losses with miscarriage complications in 2017-2018
Slide 4: Career Trajectory: U.S. Open Victory and Pre-Crisis Performance (2019-2023)
- 2019: U.S. Open Victory: U.S. Open Major Championship win at Pebble Beach established elite status in professional golf
- 2020-2022: PGA Tour Presence: Sustained presence on the PGA Tour with consistent top-25 finishes demonstrating competitive excellence
- 2023 Pre-Diagnosis: Competed in 24 events, made 18 cuts with six top-25 finishes maintaining professional standards
- Physical Condition: No prior neurological health concerns documented before diagnosis period
- Career Position: Ranked among golf's upper echelon with significant earnings and tournament success achievements
Slide 5: Timeline Overview: May 2023 to Present - From Discovery to Triumph
- May 2023: Routine MRI reveals unexpected brain lesion pressing on cranium
- May-September 2023: Four-month treatment attempt with medication management
- August 30, 2023: Public announcement of surgical decision
- September 18, 2023: Craniotomy surgery performed with majority of tumor removed
- January 2024: Return to PGA Tour competition at Sony Open
- 2025: PTSD diagnosis formally recognized
- March 2026: Houston Open victory - first tournament win post-surgery
Slide 6: The Discovery: Initial Medical Diagnosis (May 2023) and Diagnostic Process
- Routine Medical Imaging: MRI conducted for general health assessment as part of preventive medical care
- Unexpected Finding: Brain lesion identified pressing directly on neural tissue, revealed during imaging examination
- Critical Lesion Location: Located in critical cranial area near vision and motor control centers, requiring immediate medical evaluation
- Differential Diagnosis: Likely benign meningioma or non-malignant tumor classification based on initial imaging analysis
- Initial Symptoms: Cognitive fog, focus difficulties, and unexplained fatigue initially managed with medication for four months
Slide 7: Understanding the Brain Lesion: Medical Characteristics and Classification
- Tumor Type Classification: Benign lesion (non-cancerous growth) with favorable prognosis
- Pathology: Meningioma classification arising from brain's protective membranes
- Anatomical Location: Positioned on lateral skull area with proximity to critical neurological structures
- Size Consideration: Lesion large enough to create compressive effects on adjacent brain tissue
- Growth Trajectory: Progressive enlargement necessitating intervention
- Functional Impact: Pressure effects creating neurological symptoms affecting cognition and motor control
Slide 8: Brain Tumor Diagnosis: Type, Risk Profile, and Clinical Significance
- Benign Tumor Classification: Non-malignant nature with favorable long-term prognosis, indicating absence of cancerous characteristics and potential for positive patient outcomes
- Meningioma Characteristics: Typically slow-growing, encapsulated lesions originating from meningeal layers, well-defined borders that facilitate surgical separation from healthy tissue
- Compressive Neuropathy: Mass effect on brain tissue creating functional neurological impairment, producing symptoms through mechanical pressure rather than cellular invasion
- Surgical Necessity: Growth and symptom progression mandated intervention despite benign status, surgical removal essential to prevent further neurological deterioration
- Risk Stratification: Location near motor and visual cortices created significant surgical complexity, requiring meticulous operative planning to preserve critical neurological functions
- Prognostic Advantage: Benign classification offered hope and favorable outcome potential, providing reassurance regarding long-term survival and quality of life prospects
Slide 9: Pre-Surgical Symptoms: Cognitive and Physical Manifestations Over Four Months
- Cognitive Symptoms: Memory lapses, difficulty maintaining focus during competition, mental fatigue disproportionate to activity level
- Golf-Specific Impacts: Unable to recall which club to use, delayed decision-making during play
- Psychological Burden: Four-and-a-half months of daily death anxiety and catastrophizing thoughts
- Fear Escalation: Every activity (driving, flying) triggered existential dread and mortality preoccupation
- Physical Manifestations: Unexplained fatigue, stamina difficulties, and performance decline despite elite skill level
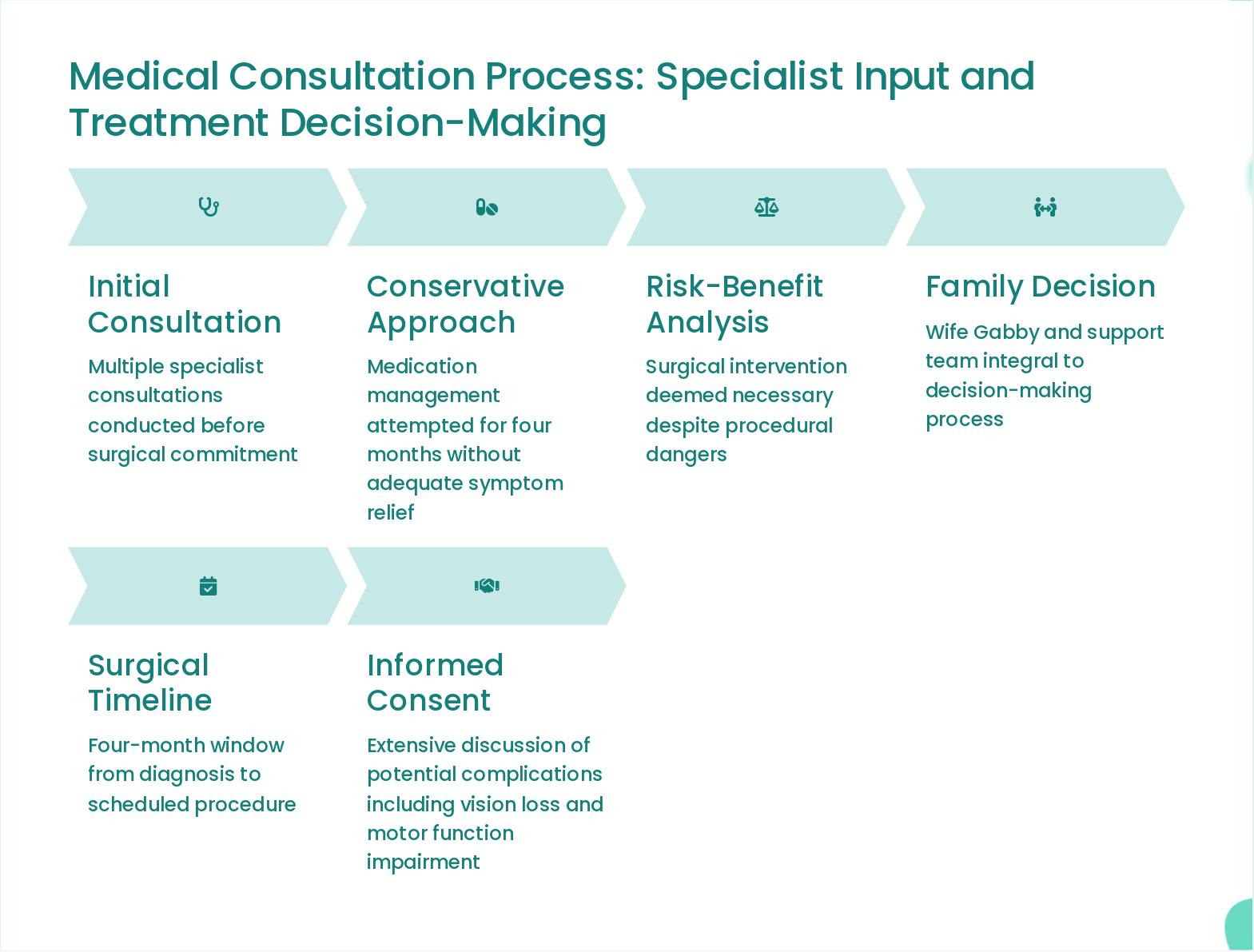
Slide 10: Medical Consultation Process: Specialist Input and Treatment Decision-Making
- Initial Consultation: Multiple specialist consultations conducted before surgical commitment
- Conservative Approach: Medication management attempted for four months without adequate symptom relief
- Risk-Benefit Analysis: Surgical intervention deemed necessary despite procedural dangers
- Family Decision: Wife Gabby and support team integral to decision-making process
- Surgical Timeline: Four-month window from diagnosis to scheduled procedure
- Informed Consent: Extensive discussion of potential complications including vision loss and motor function impairment
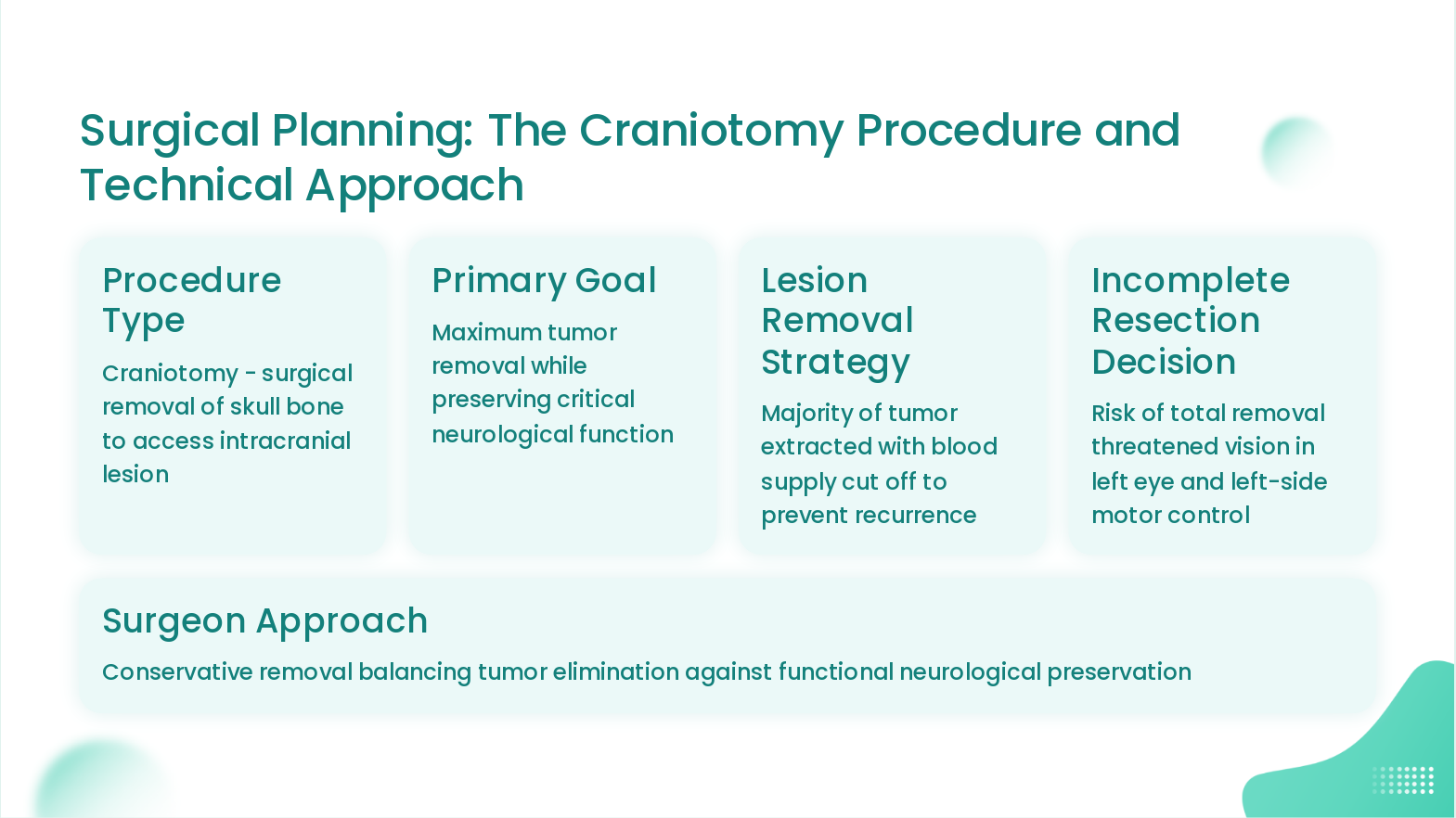
Slide 11: Surgical Planning: The Craniotomy Procedure and Technical Approach
- Procedure Type: Craniotomy - surgical removal of skull bone to access intracranial lesion
- Primary Goal: Maximum tumor removal while preserving critical neurological function
- Lesion Removal Strategy: Majority of tumor extracted with blood supply cut off to prevent recurrence
- Incomplete Resection Decision: Risk of total removal threatened vision in left eye and left-side motor control
- Surgeon Approach: Conservative removal balancing tumor elimination against functional neurological preservation
Slide 12: September 18, 2023: Surgical Execution and Intraoperative Outcomes
- Surgical Date: September 18, 2023 - approximately four months post-diagnosis
- Procedure Scope: Extensive craniotomy requiring skilled neurosurgical team expertise
- Bone Removal: Baseball-sized opening created in skull lateral wall for lesion access
- Closure Method: 30 surgical staples required to secure skull bone closure post-extraction
- Intraoperative Success: Majority of tumor mass successfully removed during procedure
- Strategic Outcome: Some residual tumor retained to protect vision and motor pathways
Slide 13: Surgical Risks and Mitigation Strategy: Balancing Cure Against Functional Preservation
- Primary Risk: Vision Loss: Vision loss in left eye from surgical tract proximity to optic pathways requiring careful surgical planning
- Secondary Risk: Motor Impairment: Left-side motor function impairment including potential limb paralysis from neural structure involvement
- Risk Mitigation: Incomplete Resection: Incomplete resection chosen strategically to preserve critical neural structures and maintain function
- Surgeon Communication: Honest discussion of incomplete removal with patients to maintain neurological integrity and trust
- Informed Trade-off: Accepting residual tumor burden to preserve sensory and motor function and quality of life
- Intraoperative Monitoring: Real-time neurological assessment during complex procedure to detect and prevent functional damage
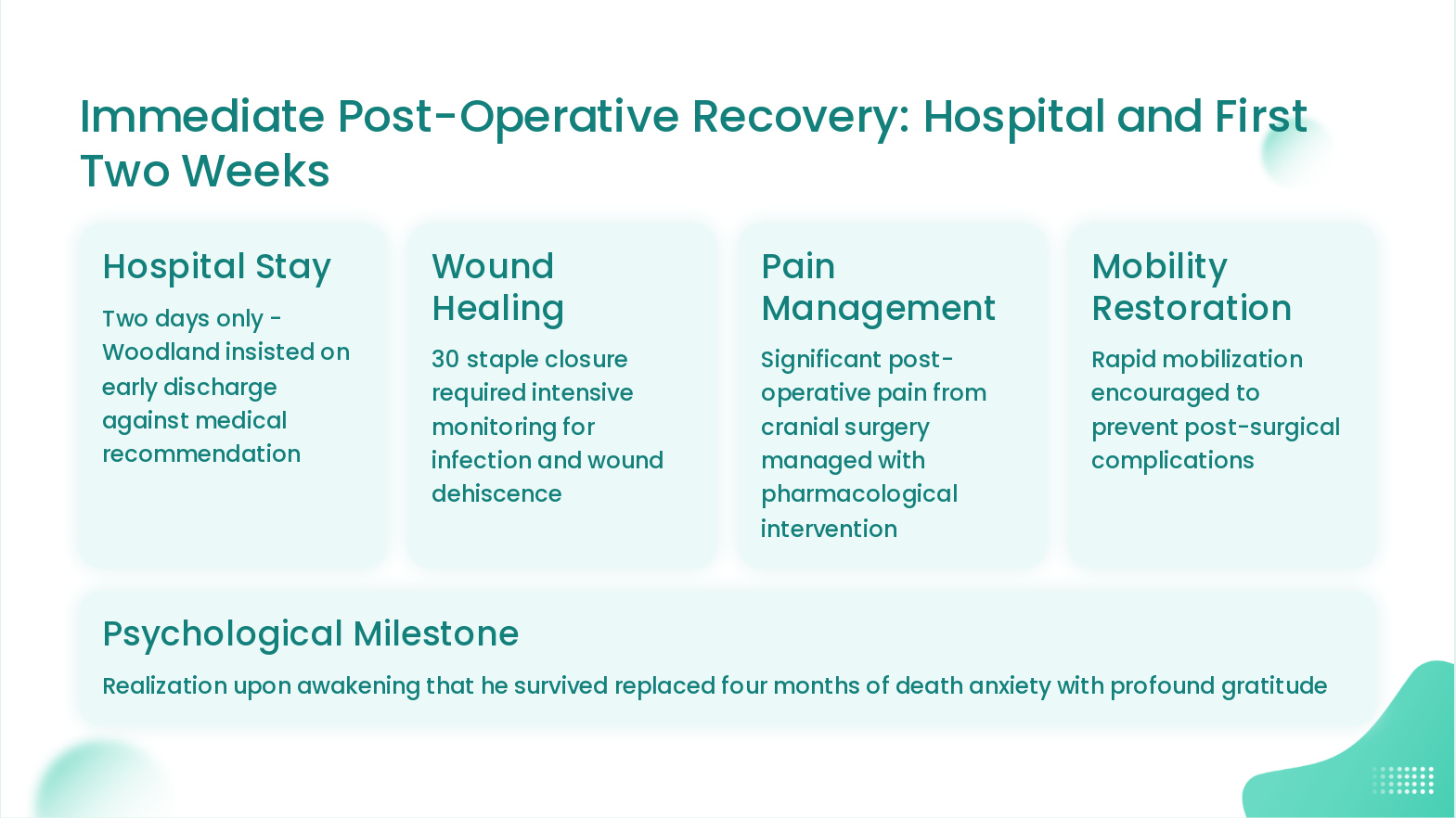
Slide 14: Immediate Post-Operative Recovery: Hospital and First Two Weeks
- Hospital Stay: Two days only - Woodland insisted on early discharge against medical recommendation
- Wound Healing: 30 staple closure required intensive monitoring for infection and wound dehiscence
- Pain Management: Significant post-operative pain from cranial surgery managed with pharmacological intervention
- Mobility Restoration: Rapid mobilization encouraged to prevent post-surgical complications
- Psychological Milestone: Realization upon awakening that he survived replaced four months of death anxiety with profound gratitude
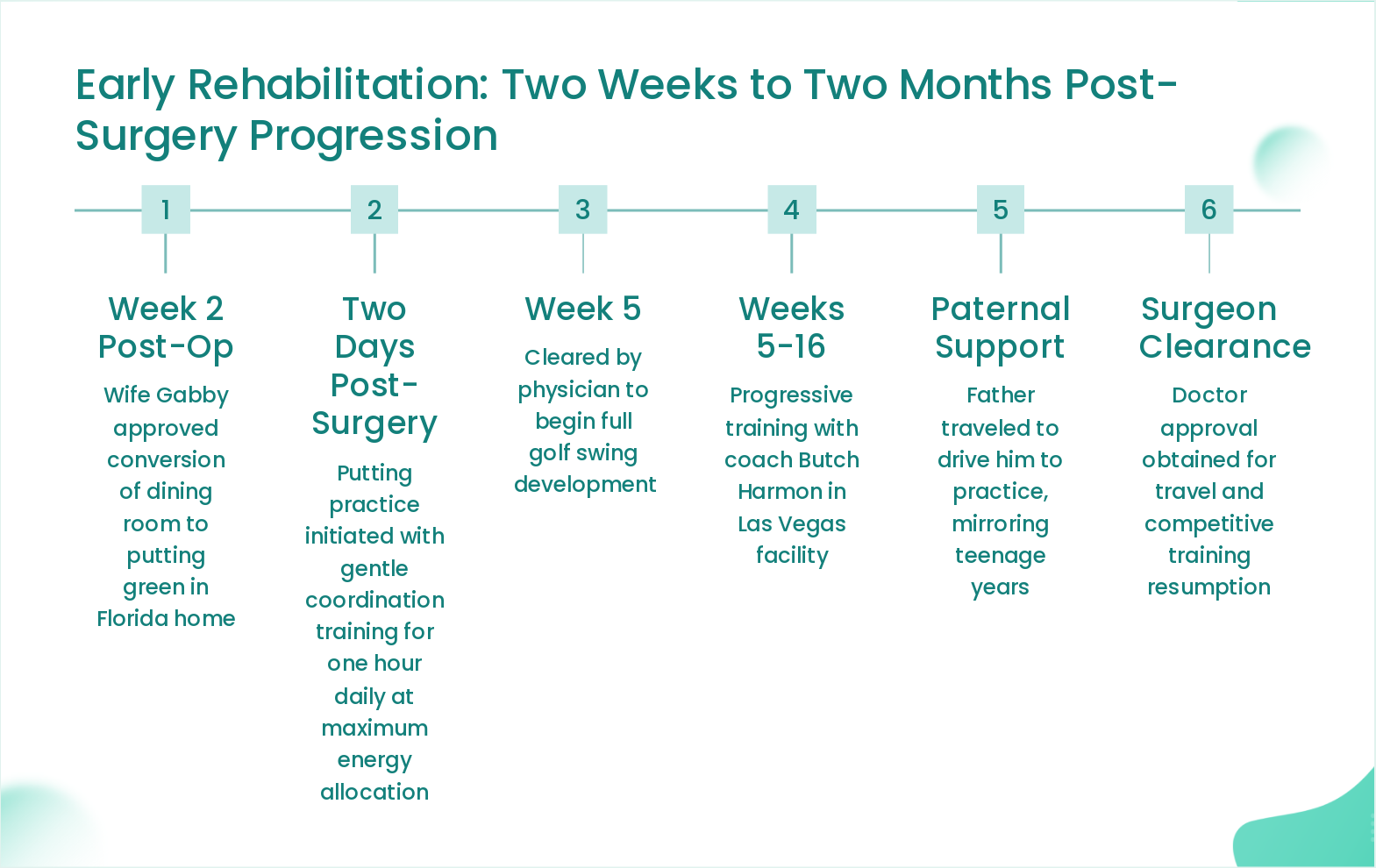
Slide 15: Early Rehabilitation: Two Weeks to Two Months Post-Surgery Progression
- Week 2 Post-Op: Wife Gabby approved conversion of dining room to putting green in Florida home
- Two Days Post-Surgery: Putting practice initiated with gentle coordination training for one hour daily at maximum energy allocation
- Week 5: Cleared by physician to begin full golf swing development
- Weeks 5-16: Progressive training with coach Butch Harmon in Las Vegas facility
- Paternal Support: Father traveled to drive him to practice, mirroring teenage years
- Surgeon Clearance: Doctor approval obtained for travel and competitive training resumption
Slide 16: Return to Golf Milestones: Progressive Training Timeline (September 2023 - January 2024)
- Two Days Post-Surgery: Putting practice initiated in home setting
- Week 5: Full golf swing development cleared by physician
- Weeks 5-16: Progressive training with elite coach Butch Harmon oversight
- Pre-Return Assessment: Comprehensive doctor evaluation confirming neurological recovery and stamina readiness
- Sony Open Preparation: First PGA Tour return planned for January 2024 – four months post-surgery
- Training Completion: Physician confirmation of readiness for tournament-level professional competition
Slide 17: The Visible Scar: Physical Recovery and Aesthetic Considerations
- Scar Location: Lateral skull beneath hair line at primary surgical site
- Scar Formation: Baseball-sized opening closure left permanent surgical scar marking procedure
- Visual Prominence: Typically concealed by hair during tournaments; visible under short hair
- Recovery Timeline: Scar maturation and fading progression progressed substantially over months
- Psychological Significance: Visible reminder of trauma created daily awareness of surgical experience
- Symbolic Transformation: Scar became symbol of survival and resilience rather than source of shame
Slide 18: Psychological Aftermath: PTSD Diagnosis and Recognition (2025-2026)
- Formal diagnosis: Post-traumatic stress disorder (PTSD) formally rendered approximately one year post-surgery
- Diagnostic criteria: Met established neurological trauma-related PTSD classification standards
- Onset recognition: Emotional and anxiety symptoms persisted despite complete physical recovery
- Professional assessment: Medical and psychological professionals independently confirmed PTSD diagnosis
- Etiological basis: Four months of death anxiety followed by brain surgery trauma created lasting psychological injury
- Neurobiological sequelae: Neurological trauma created lasting neurological anxiety patterns requiring management
Slide 19: Hypervigilance and Anxiety Manifestations: Daily Psychological Burden
- Extreme Startle Response: Hypervigilance symptom characterized by intense physiological reactions when approached from behind during any activity, creating constant alertness
- Environmental Triggers: Walking scorers, caddie proximity, and unexpected crowd sounds create acute anxiety spikes and heightened threat perception
- Cognitive Disruption: Walkers approaching from behind cause complete loss of focus and significant memory lapses, impairing task execution
- Dissociative Symptoms: Blurred vision and dissociation manifest during triggered anxious moments, creating detachment from present reality
- Executive Dysfunction: Unable to execute golf shots or make rational decisions when triggered, resulting in complete behavioral paralysis
- Accommodation Requirement: Caddie instructed to prevent anyone approaching from behind—ongoing security requirement essential for activity participation
Slide 20: Emotional Struggles During Competition: Crying and Breakdown Episodes
- FedExCup Fall Tournament: Hypervigilance episode demonstrated severe competition-related breakdown during the Napa, California event, revealing significant psychological stress responses triggered by high-pressure competition.
- Fairway Incident: Unable to execute shot despite turn to play - complete executive function collapse, indicating inability to maintain composure and decision-making capabilities during critical moments.
- In-Round Coping: Multiple bathroom visits during round for private crying episodes, demonstrating emotional overwhelm that requires isolation and temporary withdrawal from competitive play.
- Post-Round Collapse: Crying in scoring trailer and emotional isolation in vehicle after play, revealing sustained emotional distress extending beyond the competitive round into recovery periods.
- Frequency Pattern: Multiple days when anxiety symptoms overwhelmed emotion management capacity, indicating recurring and persistent emotional dysregulation across consecutive competitive events.
- Exhaustion Level: Emotional toll created daily struggle between competitive commitment and mental health preservation, reflecting the significant cost of pursuing athletic goals amid psychological challenges.
Slide 21: Support Systems: Family, PGA Tour, and Medical Team Collaborative Recovery
- Family Support: Wife Gabby, father, and three children (Jaxson, Maddox, Lennox) providing primary emotional foundation and unconditional love throughout the recovery journey
- Professional Caddie: Brennan Little provided on-course support and security oversight, ensuring a safe and stable environment during competitive play
- PGA Tour Accommodation: Organization implemented security protocols to manage triggering situations and provide structural support for the recovery process
- Peer Support: Fellow players, particularly Ryder Cup teammates, provided crucial emotional acceptance and meaningful connection during difficult moments
- Veteran Connections: Conversations with military veterans struggling with PTSD normalized experience and provided perspective from those with similar challenges
- Mental Health Professionals: Therapy and psychiatric support addressed trauma-related symptoms systematically and helped develop healthy coping mechanisms
Slide 22: Return to Competition: January 2024 Sony Open and Early Tournament Results
- Sony Open at Waialae Country Club: First PGA Tour event following brain surgery in January 2024
- Timeline Significance: Four months post-surgery, four months post-initial diagnosis
- Course Selection Strategy: Flat, low-stress course deliberately chosen for psychological and physical return
- Coach Assessment: Butch Harmon's perspective: "He got a mulligan in life, a mulligan in his career"
- Baseline Evaluation: Early results provided crucial indication of recovery trajectory and capability
- Professional Significance: Public demonstration of return to profession and resilience commitment to PGA Tour
Slide 23: Breakthrough Victory: Houston Open 2026 and Symbolic Triumph
- Tournament Achievement: Houston Open 2026 victory—approximately 2.5 years post-surgery, marking an extraordinary return to competitive excellence
- Performance Outcome: Victory by five shots demonstrating elite-level competitive ability restoration and dominance on the golf course
- Career Milestone: Fifth PGA Tour title—first major victory since 2023 brain surgery trauma, cementing professional redemption
- Symbolic Significance: Transformed suffering and recovery journey into peak professional achievement, embodying triumph over adversity
- Neurological Vindication: Proved neurological recovery and mental resilience sufficient for championship-level performance under pressure
- Broader Impact: Inspired others battling similar neurological and psychological challenges—powerful testimony to human resilience